Necrotising fasciitis - know the signs and potentially save a life!
Have you heard of necrotising fasciitis?
No? Don’t worry – you’re not alone.
This post has no absolutely information about our core business of commercial cleaning - but is potentially one that could help save a life.
Necrotising fasciitis is a rare, but life-threatening infection also known as the “flesh eating disease.” Even with treatment, it is estimated that 1 or 2 in every 5 cases are fatal. There are only circa 500 confirmed cases across the entire United Kingdom each year.
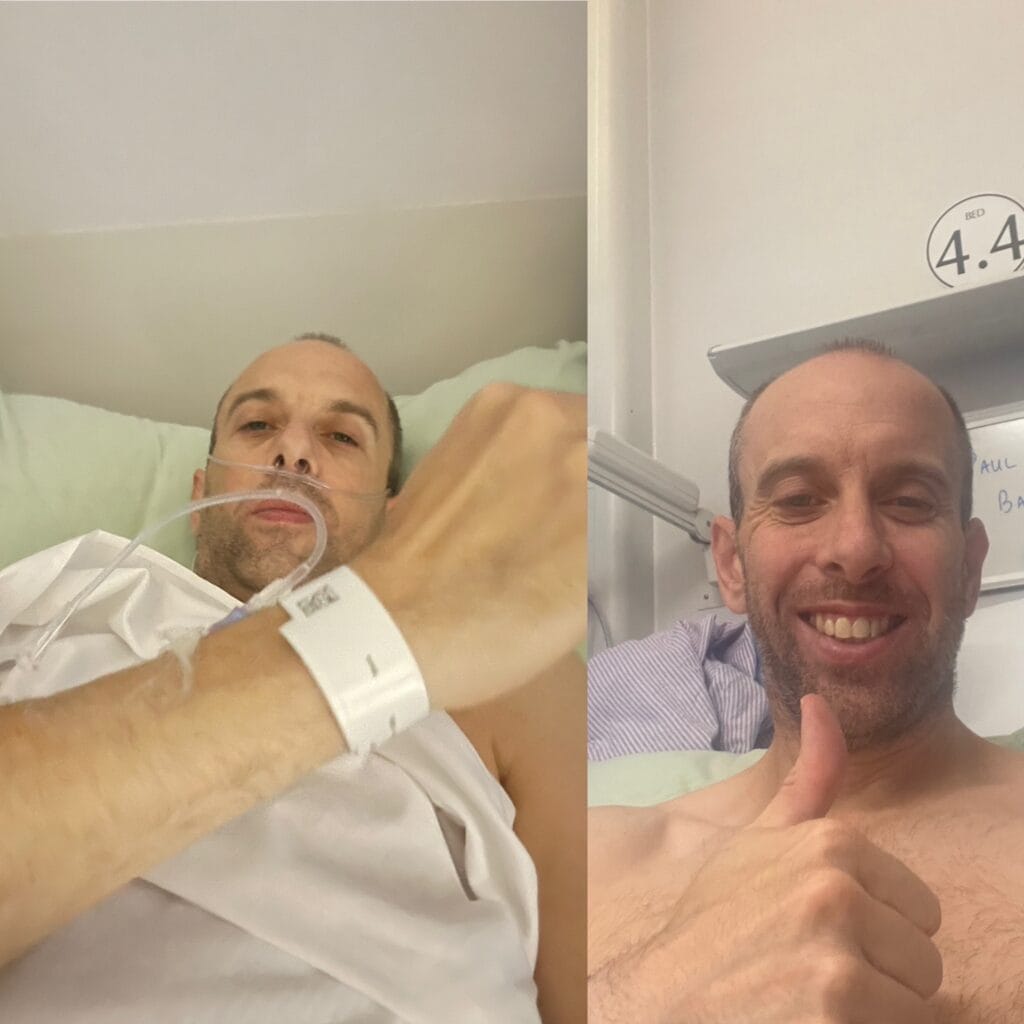
One of our founding Directors, Paul Barrett, caught this life threatening infection in November 2021. This is Paul’s story of what happened when he caught necrotising fasciitis, to try and raise awareness about this lethal infection.
Paul's story - surviving necrotising fasciitis
“It was 19th November 2021. I was living with my husband Daniel in our new home and had only been there two weeks. I went to bed feeling fine and woke around 3am. I was freezing cold, yet I was sweating profusely, and the bed was soaked. Soaked from my sweat to the degree that Daniel had to get multiple towels for me to lay on.
I felt awful, and assumed it was Covid. I had previously had Covid some months before and couldn’t think of anything else it could be.
I hadn’t eaten anything that I could think would cause food poisoning and had never heard of necrotising fasciitis.
The following morning and the next two days I felt weak and was going from hot to cold.
Daily covid tests were negative, but I was sick a handful of times and felt achy over my body – typical signs of Covid as per the NHS website.
A couple of sleepless nights passed feeling the same, with towels needed each night for profuse sweating.
Around day three, my left leg began aching. I assumed this was because I had pulled a muscle from tossing and turning in bed all night with the sweats and not being able to sleep. There was absolutely nothing visible on my leg, so I suspected simply a slightly pulled muscle.
We were due to go on holiday a couple of days later, so we decided it was best to call 111 to get some advice. They called me back within about 30 minutes after I logged the call, and due to the leg and other symptoms described, I was advised to attend my local hospital A&E department to get checked out.
By the time we arrived at hospital, I was now struggling to walk on my left leg, was sweating and kept feeling as though I was going to faint. These symptoms ramped up very quickly.
After initial screening at hospital, a blood test was taken.
I am no doctor (as will be clear from my next description), but even I could tell things were bad next. When you have a blood test to check for infection levels, the result is scored with a number (with zero being no infection).
The doctor looking after me explained that anything scoring 5 or above is an infection requiring treatment, and anything over 50 would be considered a high level of infection.
I was then told that my infection count was over four hundred!
I was immediately admitted to the majors ward, where I was attached to various machines, and fluids and medicines were pumped into me.
I could now not lift my left leg up off the bed. I didn’t know what was going on and if I would be able to move or use my leg again.
Further tests were ongoing, but no-one could work out what the infection was. Over the next few days in hospital my infection level ‘score’ increased to over 500 (ten times the number considered a high infection). I lost use of my left leg, and I was naturally fearing for my life.
Due to Covid, the opportunity for Daniel to visit me was limited to once a day after a few days, after no visits being possible initially.
I must have seen over twenty doctors / consultants over the next few days. An MRI scan showed that I had a large infection in my left leg, but this obviously couldn’t identify exactly what the infection was.
Everything changed when one surgeon came to assess me around 10pm one evening early December. This surgeon was called Mr Christie Swaminathan, and it turns out he was the person that saved my life.
Mr Swaminathan (pictured above) identified this illness as what he believed to be an extremely rare and very serious infection – necrotising fasciitis.
Mr Swaminathan was clear but very factual. I was under no doubt this was life threatening, and that I had to undergo emergency surgery to remove the infected tissue from my leg.
“When? In the morning?” was my question.
“No, as soon as the current patient in theatre comes out. This cannot wait until the morning – we are against the clock now” was his reply.
It was so serious that I was operated in the early hours that night. I was told that it was likely I would need several operations over the next few days – each removing more tissue from my leg until the infection was fully removed.
I was taken to theatre, where I was told I may wake up in intensive care if the operation didn’t go as hoped. Terrifying.
The next thing I remember is waking up in recovery. I was told the operation appeared to have gone well.
I tried to move my left leg tentatively – I felt no pain due to the strong pain relief medication still being present throughout my body, and I could move and lift my leg for the first time in days.
I cried with happiness. I knew I had a long way to recovery, but it appeared my life was saved.
The next day the pain was back and partly managed with pain relief, but it couldn’t fully control the post operation pain. I could still move my left leg, but it was weak and I couldn’t weight bear.
I was connected with a tube to a suction machine, drawing fluids off the wound 24/7 to keep it dry and sterile. Daily dressing changes were so painful when changed by staff due to the location of the wound, and peeling off the wound which had to be kept wide open, in case further operations were needed, to remove more tissue from my leg.
The next couple of weeks in hospital I underwent various processes including physiotherapy.
I would exercise to try and get strength back in my leg. I couldn’t walk to the toilet – all the things you take for granted.
I was discharged home finally on 16th December 2021, with a portable suction machine and tubing connected to me 24/7 for the next two months. Daily visits to home from nurses for assessment and dressing changes continued, with great support from Daniel.
A month or so later I got a letter from the hospital and the infection was confirmed as having been necrotising fasciitis after being tested in the hospital laboratory.
But, being connected to the machine and unable to move much didn’t matter at all – I was alive. I have survived necrotising fasciitis. I was a survivor – unlike sadly a number of other people I have read about since researching this lethal infection more.
Should I have gone to hospital or sought advice sooner? Yes. Hindsight is a wonderful thing. I would never want to waste anyone’s time, especially not our wonderful NHS staff.
Had Covid never existed, I dare say I would have also sought advice sooner.
On Tuesday 24th January 2023 I met Mr Christie Swaminathan for a (just over) one year follow up. I immediately recognised him; I thanked him for saving my life and cried. It bought it all back.
Interestingly, I was told that my hospital had only seen two further cases of necrotising fasciitis since my admission 13 months earlier – it really is rare.
I have now been fully discharged from the hospital system and am back to normal (as normal as I get anyway!), with a scar as a daily remind me of what happened.
I hope you found this insight into my experience of necrotising fasciitis and my experience useful and insightful. Please do share – the more people that read this the better. Please do also click here to learn more about NHS advice around symptoms, treatments, and the outlook on this infection”.
Symptoms of necrotising fasciitis
The symptoms of necrotising fasciitis develop quickly over hours or days.
They may not be obvious at first and can be similar to less serious conditions, such as flu, gastroenteritis or cellulitis.
Early symptoms can include:
- A small but painful cut or scratch on the skin
- Intense pain that's out of proportion to any damage to the skin
- A high temperature (fever) and other flu-like symptoms
- Diarrhoea and vomiting
If left untreated, the necrotising fasciitis infection can spread quickly through the body and cause symptoms such as dizziness, weakness and confusion.
If in doubt, please seek emergency medical advice at this stage – please don’t delay!
When to get medical help
Necrotising fasciitis is a medical emergency that requires immediate treatment.
Go to your nearest A&E department as soon as possible if you think you have it.
Call 999 for an ambulance if you're too unwell to get yourself to A&E.
The Lee Spark necrotising fasciitis foundation was established in 2000 by Doreen Cartledge following the loss of her son to necrotising fasciitis.
Click here to visit the Lee Spark Foundation website
You can click here to return to our website home page.